Breast Thermography
I would like to have a breast thermography screening. What is the protocol?
- Call 410-864-8270 to schedule an appointment, or go online to Insight-Holistic.com.
- The day of your appointment avoid exercise, deodorant, creams or oils on your skin.
- Undressing, scanning and redressing takes about 15 minutes.
- Your scan will be reviewed byu a medical doctor whis os Board Certified to interpret thermograph images,
- You will receive the results of your scan in about 7-10 days via email.
- A follow up scan is necessary 3-5 months after your first scan to establish a base line. Scans are yearly thereafter.
Breast Thermography Screen
Thermography is new to most people, especially for the application of breast health evaluation. Thermography has been used for over forty years in both the medical and industrial professions.
With industrial applications, fire fighters use thermography to detect heat behind walls; building inspectors can determine if heat is escaping through cracks in the wall. Veterinarians have used thermography on horses looking for inflammation from broken bones. And airport and government officials used thermography to detect if someone had a fever as they walked through the scanner during the swine flu pandemic in 2009.
What is Thermography?
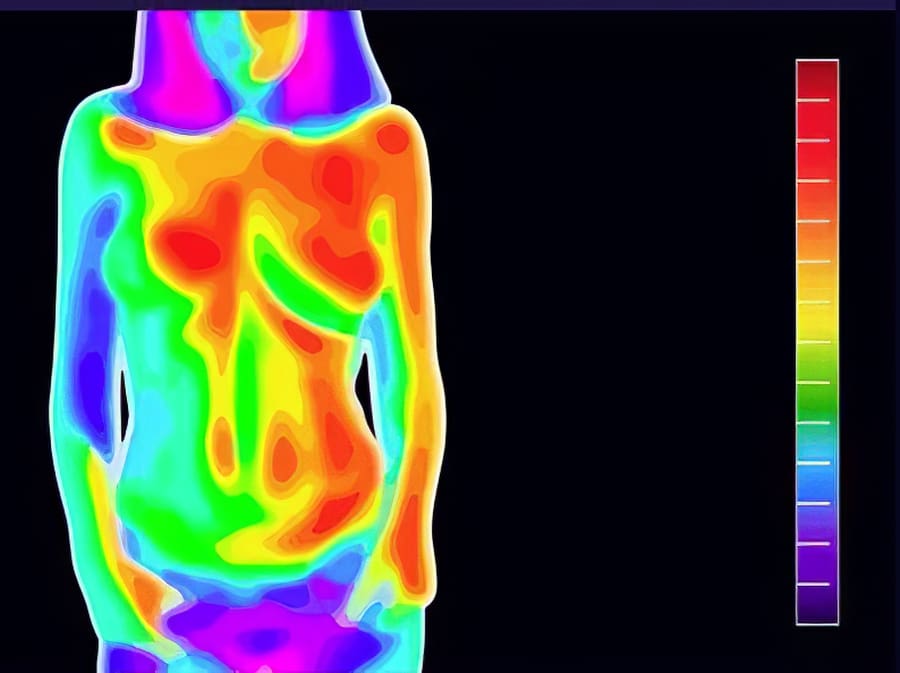
Thermography is also known as Digital Infrared Thermal Imaging (DITI). Simply defined, thermography is the detection of heat. A thermography technician manipulates the cameras computer to view the breast. The computer displays blue as cold and red as hot. Yellow and green represent temperatures in between hot and cold. Once she has the correct variance of temperature, she snaps the picture.
Both breasts should have approximately the same temperature and therefore same color. Variations in color or unequal distribution of color must be interpreted by a medical doctor specially trained in reading thermographic images. Not all variation in color is a reason for concern.
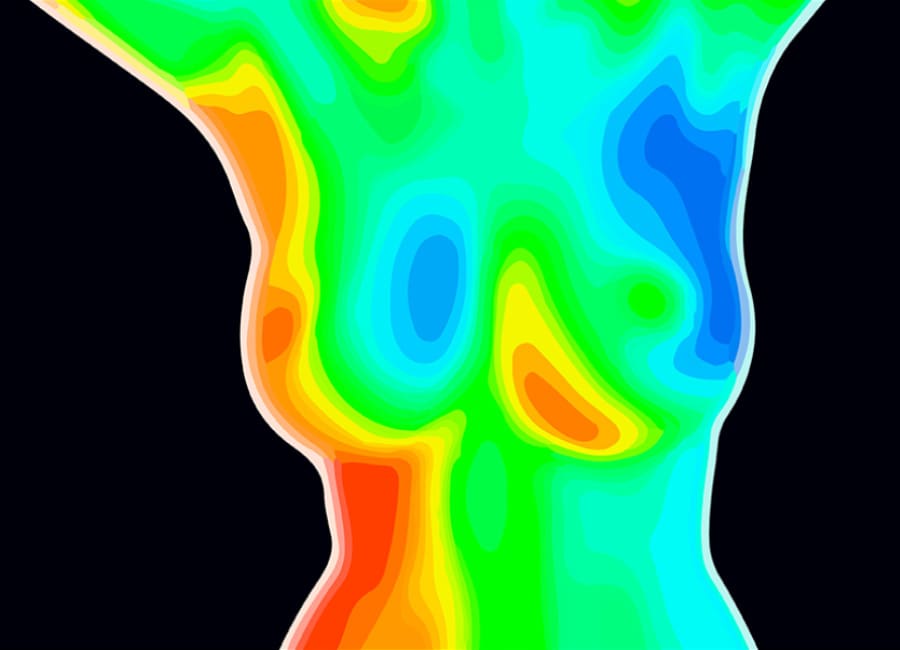
Why is DITI so useful for breast screening?
As mentioned above, red means heat. If there is a red dot in the left breast for example, and that dot becomes enlarged as seen on future scans, this indicates the presence of heat development. Blood is hot and cancer cells need blood to divide and grow. If these are inflammatory cancer cells, thermography is able to detect the physiologic change years before mammography is able to detect a mass.
Does insurance cover thermography?
Not at this time.
Who will take the thermography of me?
A female certified technician operates the camera for female and male patient’s having breast thermography.

Should I Stop having mammograms?
No. Thermography is a screening tool. The purpose is to detect physiologic change. The purpose of a mammogram is to detect the presence an anatomic mass. A suitable analogy is weather Doppler. Discovering a storm brewing hundreds of miles off the coast of Florida is thermography. Once the storm hits land, we call it mammography. Thermography is considered a favorable adjunct to mammography.
What are the risks to thermography?
There are no risks. There is no compression, no radiation and no invasive procedure. The procedure is painless. You will stand about four feet from the camera with your arms positioned on your head. The technician manipulates the camera and in several minutes the test is over.
Does the medical profession recognize thermography?
Yes. Although, thermography is not part of main stream breast care. Most medical professionals are not familiar with thermography as a viable screening tool.
In the 1970’s thermography was used medically and was covered by insurance. The findings were promising, but they were unable to substantiate what they saw on thermography. In the opinion of the doctors and researchers there were too many false positive; so they did away with thermography screenings. Years later, many of the initial females screened had developed breast cancer. The doctors looked back and realized those were not false positives. It was at that point they realized thermography was actually more advanced than the current testing systems. Today, thermography continues to be a front runner in early detection of physiologic change in the body.
